Male Hormone Restoration
Why is it Important to Maintain Balanced Male Hormones?
 Maintaining balanced hormone levels is essential to overall health. Unfortunately, testosterone levels decline in men as they age. Most men know that testosterone is important for sexual function, but research indicates that it is critical for so much more: maintaining cognitive function and a healthy body weight, improving insulin sensitivity and glucose metabolism, promoting heart health, and more. In addition, the ratio of testosterone to estrogen appears to be a strong indicator of mortality outcomes in men with heart disease.
Maintaining balanced hormone levels is essential to overall health. Unfortunately, testosterone levels decline in men as they age. Most men know that testosterone is important for sexual function, but research indicates that it is critical for so much more: maintaining cognitive function and a healthy body weight, improving insulin sensitivity and glucose metabolism, promoting heart health, and more. In addition, the ratio of testosterone to estrogen appears to be a strong indicator of mortality outcomes in men with heart disease.
Testosterone levels are affected by several other hormones and enzymes, such as dehydroepiandrosterone (DHEA) (a precursor to testosterone and estrogen), aromatase (an enzyme that converts testosterone to estrogen), and sex hormone-binding globulin (SHBG) (a glycoprotein that binds testosterone). Comprehensive hormone testing is recommended before implementing any replacement therapy.
Natural alternatives to hormone replacement, such as nettle root and zinc, may support healthy testosterone levels.
What Factors Can Lead to Low Testosterone Levels?
- Age
- Increased body fat
- Oxidative damage
- Declining levels of precursors, such as DHEA
- Poor nutritional status and liver function
Why is it Important to Get Hormone Levels Tested?
 Comprehensive hormone testing is necessary to obtain an accurate overview of your hormone balance. Both free and total testosterone levels are important, as well as estrogen levels to determine ratios. Hormone levels will vary widely between people, so it is important to repeat tests over time to establish whether levels are declining or changing. ONLY after comprehensive testing can one decide whether hormone replacement therapy is a good choice, and ONLY with the guidance of a healthcare professional.
Comprehensive hormone testing is necessary to obtain an accurate overview of your hormone balance. Both free and total testosterone levels are important, as well as estrogen levels to determine ratios. Hormone levels will vary widely between people, so it is important to repeat tests over time to establish whether levels are declining or changing. ONLY after comprehensive testing can one decide whether hormone replacement therapy is a good choice, and ONLY with the guidance of a healthcare professional.
Do High Testosterone Levels Increase the Risk of Prostate Cancer?
No. As of the time of this writing, the scientific literature does not support an association between high testosterone levels and an increased risk of prostate cancer.
What are Natural Ways to Boost Testosterone Levels?
Aside from hormone replacement therapy, there are many natural ways to support testosterone levels and healthy male function:
 Zinc. Zinc is essential for many aspects of male reproductive function, from testosterone metabolism to sperm motility.
Zinc. Zinc is essential for many aspects of male reproductive function, from testosterone metabolism to sperm motility.- DHEA. As a precursor to testosterone, adequate DHEA levels are required for healthy testosterone production. DHEA levels tend to decline with age.
- Tribulus. Protodioscin, an active ingredient in Tribulus terrestris (or puncture vine), may convert to DHEA in the body. It has a reputation as an aphrodisiac, and animal studies seem to confirm its ability to boost sexual function.
- Antioxidants. Antioxidant supplements, including vitamins A and E and selenium, have been shown to boost testosterone production in men.
- Chrysin. This bioflavonoid naturally inhibits aromatase, and thus may reduce the conversion of testosterone to estrogen. Its bioavailability may be boosted by taking with piperine (black pepper extract).
- Nettle root. Lignans in nettle root may prevent SHBG from binding testosterone, which may boost free testosterone levels. Nettle root is often used to relieve benign prostatic hyperplasia (BPH) symptoms.
- Muira puama. Muira puama may improve sexual performance in men who have loss of libido.
- Indole-3-carbinol (I3C). I3C, found in many cruciferous vegetables, may protect the prostate from harmful estrogen metabolites.
- Pygeum. Pygeum has been used to relieve BPH symptoms in Europe since the 1960’s. Pygeum may prevent the conversion of testosterone to a metabolite that can exacerbate BPH.
- Saw palmetto. Saw palmetto is a popular supplement for prostate health. Its clinical benefits include reduced nighttime urinary urgency and less discomfort from urination symptoms.
- Other natural products such as quercetin, fish oil, maca, L-carnitine, protein, and more may help support healthy testosterone levels and male functions.
The significance of testosterone for male sexual function is apparent to most Life Extension customers. New insights, however, underscore the critical role testosterone plays in maintaining youthful neurological structure, alleviating depression, as well as inducing fat loss in those who are unable to reduce body weight regardless of diet and exercise.
 Recent studies have demonstrated that low testosterone in men is strongly associated with metabolic syndrome, type 2 diabetes, cardiovascular disease,1 and an almost 50% increase in mortality over a seven-year period.2
Recent studies have demonstrated that low testosterone in men is strongly associated with metabolic syndrome, type 2 diabetes, cardiovascular disease,1 and an almost 50% increase in mortality over a seven-year period.2
Restoring testosterone to youthful ranges in middle-aged, obese men resulted in an increase in insulin sensitivity as well as a reduction in total cholesterol, fat mass, waist circumference and pro-inflammatory cytokines associated with atherosclerosis, diabetes, and the metabolic syndrome.3-5 Testosterone therapy also significantly improved erectile function6 and improved functional capacity, or the ability to perform physical activity without severe duress, in men with heart failure.7
Factors That Affect Testosterone Levels in Men
DHEA
Dehydroepiandrosterone (DHEA) is a hormone produced from cholesterol that then follows one of two pathways, both involving two-step enzymatic conversions, to yield either estrogens or testosterone. Thus, levels of DHEA can have a role in determining levels of estrogen and testosterone, though DHEA alone is seldom enough to sufficiently restore testosterone levels in aging men.
Aromatase
One of the most important factors that affect testosterone levels and the ratio between testosterone and estrogen is the aromatase enzyme. Aromatase converts testosterone to estrogen, further depleting free testosterone levels and increasing estrogen levels.
Obesity
 Obesity and associated hyperinsulinemia suppress the action of luteinizing hormone (LH) in the testis, which can significantly reduce circulating testosterone levels,8 even in men under the age of 40.9 In addition, increased belly fat mass has been correlated with increased aromatase levels.10
Obesity and associated hyperinsulinemia suppress the action of luteinizing hormone (LH) in the testis, which can significantly reduce circulating testosterone levels,8 even in men under the age of 40.9 In addition, increased belly fat mass has been correlated with increased aromatase levels.10
The vicious circle of low testosterone and obesity has been described as the hypogonadal/obesity cycle. In this cycle a low testosterone level results in increased abdominal fat, which in turn leads to increased aromatase activity. This enhances the conversion of testosterone to estrogens, which further reduces testosterone and increases the tendency toward abdominal fat.11,12
Sex Hormone-Binding Globulin
Most testosterone circulating in the bloodstream is bound to either sex hormone-binding globulin (SHBG) (60%) or albumin (38%). Only a small fraction (2%) is unbound, or "free."13
 Testosterone binds more tightly to SHBG than to albumin.14 Consequently, only albumin-bound testosterone and free testosterone constitute the bioavailable forms of testosterone, which are accessible to target tissues and carry out the actions of the essential hormone.13 Thus, the bioavailability of testosterone is influenced by the level of SHBG.
Testosterone binds more tightly to SHBG than to albumin.14 Consequently, only albumin-bound testosterone and free testosterone constitute the bioavailable forms of testosterone, which are accessible to target tissues and carry out the actions of the essential hormone.13 Thus, the bioavailability of testosterone is influenced by the level of SHBG.
Aging men experience both an increase in aromatase activity and an elevation in SHBG production. The net result is an increase in the ratio of estrogen to testosterone and a decrease in total and free testosterone levels.15 As will be discussed below, it is crucial that this skewed ratio be balanced.
Liver Function
The liver is responsible for removing excess estrogen and SHBG, and any decrease in liver function could exacerbate hormonal imbalances and compromise healthy testosterone levels. Thus, it is important that aging men also strive for optimal liver function.
Effects of Age-Related Decline in Testosterone Levels and Testosterone Therapy
The exact cause of the age-related reduction in testosterone levels is not known; it is probably the result of a combination of factors, including:
- Increasing body fat (especially belly fat, and therefore increasing aromatase activity)
- Oxidative damage to tissues responsible for the production of testosterone
- Reduction in testicular testosterone synthesis
- Declining levels of precursor molecules, such as DHEA
- Nutritional status and liver function
The consequences of declining testosterone levels are striking
Body Composition and Inflammation
 Testosterone affects fat cell metabolism and fat loss in several ways: inhibiting fat storage by blocking a key enzyme called lipoprotein lipase that is necessary for the uptake of fat into the body’s fat cells; stimulating fat burning by increasing the number of specific receptors on the fat-cell membrane that release stored fat; increasing insulin sensitivity; enhancing growth of muscle fibers; and decreasing fat deposits. All of these effects promote lean body mass and reduce fat mass.16,17 Placebo-controlled trials have demonstrated both significant increases in lean body mass and decreases in fat mass after varying courses of testosterone treatment in older men. In these studies, the greatest favorable changes in body composition were seen in participants with low baseline testosterone levels who received testosterone therapy for 12 months or longer.18
Testosterone affects fat cell metabolism and fat loss in several ways: inhibiting fat storage by blocking a key enzyme called lipoprotein lipase that is necessary for the uptake of fat into the body’s fat cells; stimulating fat burning by increasing the number of specific receptors on the fat-cell membrane that release stored fat; increasing insulin sensitivity; enhancing growth of muscle fibers; and decreasing fat deposits. All of these effects promote lean body mass and reduce fat mass.16,17 Placebo-controlled trials have demonstrated both significant increases in lean body mass and decreases in fat mass after varying courses of testosterone treatment in older men. In these studies, the greatest favorable changes in body composition were seen in participants with low baseline testosterone levels who received testosterone therapy for 12 months or longer.18
Emergent evidence suggests that maintaining youthful testosterone levels may help aging men avert a variety of inflammation-mediated disease, such as atherosclerosis and arthritis. By powerfully suppressing the activity an enzyme called 5-lipoxygenase, testosterone calms a fundamental pro-inflammatory pathway involved in the synthesis of signaling molecules known as leukotrienes.19 Leukotrienes are derivatives of the pro-inflammatory omega-6 fatty acid arachidonic acid; these molecules underlie much of the inflammatory development of asthma and bronchitis, and play a role in the pathology of cardiovascular disease and diabetes as well.20,21
In a study involving 184 men with low testosterone levels, 18 weeks of testosterone replacement therapy suppressed markers of inflammation including IL-1β, TNF-α, and C-reactive protein. Moreover, when compared to men who received a placebo control, men receiving testosterone replacement exhibited significant decreases in body weight, and body mass index (BMI), and waist circumference.22 The reduction in waist circumference indicates that testosterone reduces fat accumulation around the trunk of the body; this is particularly important since central fat mass and is strongly associated with increased susceptibility to inflammatory diseases and mortality.23
 Testosterone therapy has been shown to decrease weight and improve measures of health in men with low testosterone levels. In a non-randomized registry study of 471 obese men with hypogonadism, patients elected to receive either testosterone undecanoate injections (1,000 mg every 12 weeks) or no therapy (control group). After up to 11 years, weight decreased an average of 23 kg (51 lb, or about 20% of body weight) in the testosterone group versus a 6 kg (13 lb, or about 6% of body weight) increase in the control group. Testosterone treatment was also associated with a decrease in waist circumference of 13.3 cm compared with an increase of 6.7 cm in the control group. Finally, testosterone may have had positive effects on other health outcomes. In the control group, heart attacks occurred in 28% and stroke in 27% of men; no heart attacks or strokes were reported in the testosterone group. Deaths were also reported at a significantly lower rate in those who received testosterone compared with those who did not (8% vs. 32%).99 Importantly, the findings of this study had not yet been published in a peer-reviewed journal at the time of this writing and could change following peer review; the findings were presented at the 2020 virtual European and International Congress on Obesity.
Testosterone therapy has been shown to decrease weight and improve measures of health in men with low testosterone levels. In a non-randomized registry study of 471 obese men with hypogonadism, patients elected to receive either testosterone undecanoate injections (1,000 mg every 12 weeks) or no therapy (control group). After up to 11 years, weight decreased an average of 23 kg (51 lb, or about 20% of body weight) in the testosterone group versus a 6 kg (13 lb, or about 6% of body weight) increase in the control group. Testosterone treatment was also associated with a decrease in waist circumference of 13.3 cm compared with an increase of 6.7 cm in the control group. Finally, testosterone may have had positive effects on other health outcomes. In the control group, heart attacks occurred in 28% and stroke in 27% of men; no heart attacks or strokes were reported in the testosterone group. Deaths were also reported at a significantly lower rate in those who received testosterone compared with those who did not (8% vs. 32%).99 Importantly, the findings of this study had not yet been published in a peer-reviewed journal at the time of this writing and could change following peer review; the findings were presented at the 2020 virtual European and International Congress on Obesity.
Musculoskeletal System
Bone integrity rests upon a balance between bone formation and bone resorption, which is controlled by multiple factors—including levels of estrogen and testosterone.24,25 In a clinical trial, testosterone increased bone mineral density in elderly men.26 Testosterone supplementation also has a positive effect on muscle metabolism and strength.27 This positive effect is undiminished with age.
Central Nervous System (CNS)
 Key to aging well is an optimistic outlook on life and the ability to engage in social and physical activity. However, low levels of testosterone have been associated with depression and other psychological disorders.28 To make matters worse for aging men, many conventional antidepressant medications suppress libido. Some experts suggest that testosterone therapy might reduce the need for the antidepressant medications entirely.29,30 Furthermore, testosterone treatment often increases feelings of well-being.31
Key to aging well is an optimistic outlook on life and the ability to engage in social and physical activity. However, low levels of testosterone have been associated with depression and other psychological disorders.28 To make matters worse for aging men, many conventional antidepressant medications suppress libido. Some experts suggest that testosterone therapy might reduce the need for the antidepressant medications entirely.29,30 Furthermore, testosterone treatment often increases feelings of well-being.31
Cognition and alertness are also governed, in part, by testosterone’s effects on the CNS.32 Low testosterone levels have been shown to correlate with lower scores on various psychometric tests,33 and similar effects have been reported in men undergoing androgen (male hormone)-deprivation therapy for prostate cancer.34
Testosterone also acts as an endogenous neuroprotective agent, able to support neuron integrity against a variety of toxic insults, including oxidative stress.35,36 In addition, testosterone has been shown to reduce β-amyloid accumulation, an important pathophysiologic factor in Alzheimer’s disease.37,38
Testosterone improves neuron survival in brain regions vulnerable to neurodegenerative disease. This may explain the association of low testosterone levels in men with neurodegenerative diseases.39,40 Studies demonstrate testosterone loss occurred 5‒10 years prior to Alzheimer’s disease diagnosis. This suggests low testosterone is an important risk factor for Alzheimer’s disease.41,42 In a clinical study of 36 men recently diagnosed with Alzheimer’s disease, intramuscular testosterone treatment with 200 mg every two weeks for up to one year was associated with improvement in both overall cognitive ability as well as critical visual-spatial function.43
Glucose and Lipid Metabolism
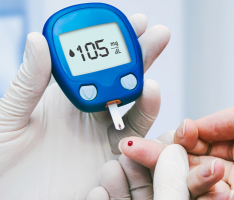 Testosterone also has been linked to metabolic function in the body. Specifically, studies have found inverse associations between the severity of metabolic syndrome, a condition characterized by excess abdominal fat, high cholesterol and high blood pressure that predisposes one for cardiovascular disease, and low plasma testosterone.18,44 A clinical study demonstrated that men with low testosterone levels are twice as insulin resistant as their counterparts with normal testosterone levels, and 90% met the criteria for the metabolic syndrome.45
Testosterone also has been linked to metabolic function in the body. Specifically, studies have found inverse associations between the severity of metabolic syndrome, a condition characterized by excess abdominal fat, high cholesterol and high blood pressure that predisposes one for cardiovascular disease, and low plasma testosterone.18,44 A clinical study demonstrated that men with low testosterone levels are twice as insulin resistant as their counterparts with normal testosterone levels, and 90% met the criteria for the metabolic syndrome.45
There also appears to be an inverse relationship between low testosterone levels and diabetes in men.46 Men with diabetes have lower testosterone levels compared to men without a history of diabetes.47 The Third National Health and Nutrition survey of 1,413 men showed that men initially ranked in the lowest one-third with respect to either free or bioavailable testosterone were approximately four times more likely to have prevalent diabetes compared with those ranked in the top one-third, after researchers adjusted the results for age, race/ethnicity, and adiposity.48
Cardiovascular Health
 While conventional thought has been that because more men die from heart attacks than women, the disparity must have something to do with testosterone. However, research is pointing out that, in fact, the opposite may be true. Low levels of testosterone appear to be correlated with several cardiovascular risk factors, including atherogenic lipid profiles, insulin resistance, obesity, and a propensity to clot.49 In addition, recent research is showing a clear relationship between low testosterone levels and increased incidence of cardiovascular disease and mortality in men.2
While conventional thought has been that because more men die from heart attacks than women, the disparity must have something to do with testosterone. However, research is pointing out that, in fact, the opposite may be true. Low levels of testosterone appear to be correlated with several cardiovascular risk factors, including atherogenic lipid profiles, insulin resistance, obesity, and a propensity to clot.49 In addition, recent research is showing a clear relationship between low testosterone levels and increased incidence of cardiovascular disease and mortality in men.2
Prostate Health
Compared to younger men, older males have much more estradiol (a potent form of estrogen) than free testosterone circulating in the body. These rising estrogen and declining androgen levels are even more sharply defined in the prostate gland.
Estrogen levels increase significantly in the prostate with age, and estrogen levels in prostate gland tissues rise even higher in men who have BPH.50-52
An important study indicates that testosterone is beneficial for the prostate gland in the vast majority of cases. In this study researchers looked at multiple parameters, including prostate volume, prostate-specific antigen (PSA) levels, and lower urinary tract symptoms in a group of men with low or low-normal testosterone levels.53 Of the 207 men studied, 187 responded favorably to testosterone treatment.
The Importance of Hormone Testing
 Millions of aging men have the dual conditions of low testosterone and high cholesterol. Conventional physicians prescribe cholesterol-lowering drugs to reduce cholesterol, when, in fact, the age-related rise in cholesterol might simply be the body's way of increasing hormone levels by supplying the raw materials necessary to make hormones.54 Researchers at Life Extension have successfully treated high cholesterol levels through a program of bioidentical hormone replacement therapy.
Millions of aging men have the dual conditions of low testosterone and high cholesterol. Conventional physicians prescribe cholesterol-lowering drugs to reduce cholesterol, when, in fact, the age-related rise in cholesterol might simply be the body's way of increasing hormone levels by supplying the raw materials necessary to make hormones.54 Researchers at Life Extension have successfully treated high cholesterol levels through a program of bioidentical hormone replacement therapy.
Life Extension believes that comprehensive tests, along with a careful physical examination, are essential in detecting hormonal imbalances in aging men.
The so-called "normal" levels of testosterone in older men reflect population averages. Life Extension believes that most aging men would prefer not to accept the loss of youthful vigor as normal. Instead, we suggest that a more valid optimal level for all men would be in the upper one-third of the reference range used for men aged 21 to 49 years, and that any supplementation should aim to restore hormone levels to that range. The current Life Extension optimal level of free testosterone is 20‒25 pg/mL.
 When measuring testosterone levels, it is critical to determine the levels of both free and total testosterone to understand the cause of any observed symptoms of deficiency.55
When measuring testosterone levels, it is critical to determine the levels of both free and total testosterone to understand the cause of any observed symptoms of deficiency.55
Because of difficulties with equipment standardization and inter-laboratory variability, it is recommended that physicians consistently use the same local laboratories and gain familiarity with the accuracy, precision and definition of normal values for the assays offered in their communities.13
It is also important to remember that blood levels of both free and total testosterone vary widely among individuals, making it difficult to establish a general baseline on which to prescribe a standardized treatment protocol. However, levels are quite consistent within individuals, and thus it is important that men have multiple tests over time to determine trends and individual thresholds for treatment.
Finally, during the initial testing, it is also imperative to test estrogen levels. Many of the unwanted effects of male hormone imbalance are actually caused by an elevated estrogen level relative to low testosterone levels (the estrogen/testosterone ratio). The Life Extension optimal level of estrogen (measured as estradiol) for aging men is 20‒30 pg/mL.
Testosterone Replacement Therapies
 Optimal testosterone treatment usually requires a physician’s prescription. Integrative physicians typically prescribe bioidentical testosterone creams (available from compounding pharmacies). Conventional physicians are more likely to prescribe prepackaged, testosterone patches and/or gels from pharmaceutical companies that have sought FDA approval for the mass commercialization of their products.
Optimal testosterone treatment usually requires a physician’s prescription. Integrative physicians typically prescribe bioidentical testosterone creams (available from compounding pharmacies). Conventional physicians are more likely to prescribe prepackaged, testosterone patches and/or gels from pharmaceutical companies that have sought FDA approval for the mass commercialization of their products.
All forms of bioidentical testosterone have the same molecular structure and will increase free and total testosterone in the blood. The major difference is that prepackaged versions could cost up to 10 times more per dose than compounded versions. Furthermore, prepackaged testosterone gels are sold only in a limited number of doses, whereas compounded testosterone can be formulated at virtually any dose the physician feels is clinically necessary and useful.
Using Hormone Replacement Wisely
If a man opts for testosterone therapy (available orally or as an injection, subcutaneous implant, topical cream, gel, or skin patch), he should keep several facts and precautions in mind57,58:
 Hormone replacement should not be initiated without comprehensive testing.
Hormone replacement should not be initiated without comprehensive testing.- The patterns and trends over time of multiple hormone levels (eg, free testosterone, total testosterone, and estrogen) determine the specific hormone replacements required.
- It may not be safe to use large amounts of testosterone in any form without also using aromatase-inhibiting supplements or medications.
- Because of the risk of worsening prostate cancer, careful screening, including a digital rectal examination and prostate specific antigen (PSA) screening, must be done before starting any hormone replacement program. However, recent research indicates that low endogenous testosterone levels may present a greater risk for prostate cancer than higher levels.59,60 If a man already has prostate cancer, however, testosterone replacement should be delayed until the underlying cancer is eradicated.
- A man contemplating hormone replacement, whether through a prescription or supplements, should work closely with a qualified physician to plan a rational treatment approach that includes continued monitoring and screening.
- There is no “one-size-fits-all” treatment. Individuals vary, and hormone replacement can be a simple or complex process and often requires careful attention to signs and symptoms, as well as laboratory testing.
Boost Testosterone and Suppress Estrogen Levels Naturally
For men who choose not to (or are advised not to) use hormone replacement therapy, nutrients can play a vital role in a comprehensive program designed to reduce the impact of aging on sex hormone production and metabolism. The following is a list of nutrients that are part of Life Extension's comprehensive male hormone restoration program.
Essential Nutrients for Optimal Testosterone Production
 Zinc. This mineral is involved in almost every aspect of male reproduction, including testosterone metabolism, sperm formation, and sperm motility.61 A prime example of the usefulness of zinc was illustrated in a study of 37 infertile men with decreased testosterone levels and associated low sperm counts.62 The men were given 60 mg of zinc daily for 45‒50 days. In the majority of patients, testosterone levels significantly increased and mean sperm count rose from 8 million to 20 million. Some men require higher levels of zinc to adequately suppress aromatase.
Zinc. This mineral is involved in almost every aspect of male reproduction, including testosterone metabolism, sperm formation, and sperm motility.61 A prime example of the usefulness of zinc was illustrated in a study of 37 infertile men with decreased testosterone levels and associated low sperm counts.62 The men were given 60 mg of zinc daily for 45‒50 days. In the majority of patients, testosterone levels significantly increased and mean sperm count rose from 8 million to 20 million. Some men require higher levels of zinc to adequately suppress aromatase.
DHEA. DHEA is an important hormone that tends to be depleted steadily with age.63 A 2006 study assessing DHEA supplementation in men of average 65 years of age found that the men experienced significant increases in testosterone and significant decreases in low-density lipoprotein.64
Tribulus. Tribulus terrestris, also known as puncture vine, contains the active ingredient protodioscin, which is reportedly converted to DHEA in the body.65 This DHEA-boosting activity may account for puncture vine’s reputation as an aphrodisiac in its native Europe and Asia. Animal studies appear to confirm the ability of tribulus to improve sexual function.66,67
 Antioxidants. One reason testosterone production may decline with advancing age is oxidative damage in the tissues that produce testosterone. A study examining the role of antioxidants in male hormone imbalance in aging men noted that antioxidant supplements (including vitamins A and E, zinc, and selenium) all supported testosterone production.68
Antioxidants. One reason testosterone production may decline with advancing age is oxidative damage in the tissues that produce testosterone. A study examining the role of antioxidants in male hormone imbalance in aging men noted that antioxidant supplements (including vitamins A and E, zinc, and selenium) all supported testosterone production.68
Natural Products to Keep Aromatase and/or Sex Hormone-Binding Globulin (SHBG) in Check
Chrysin. The bioflavonoid chrysin is a natural aromatase inhibitor.69 Bodybuilders have used chrysin as a testosterone-boosting supplement, because it minimizes the conversion of testosterone to estrogen. Although chrysin has low oral bioavailability,70 its bioavailability may be significantly enhanced by co-administration with the black pepper extract, piperine, thus enhancing its actions as an aromatase inhibitor.71
Quercetin. One study showed that red wine inhibits aromatase, thus inhibiting the conversion of testosterone to estrogen. The study attributed this effect to the quercetin and other ingredients.72
%20in%20Check.jpg) Nettle root. Lignans contained in nettle root extract may help prevent the binding of sex hormone-binding globulin to testosterone. This may help ensure that free testosterone is available for promoting male vitality and youthful sexual function.73,74 Nettle root extract is used extensively, either in combination with saw palmetto75 or by itself76 for relief of BPH symptoms.
Nettle root. Lignans contained in nettle root extract may help prevent the binding of sex hormone-binding globulin to testosterone. This may help ensure that free testosterone is available for promoting male vitality and youthful sexual function.73,74 Nettle root extract is used extensively, either in combination with saw palmetto75 or by itself76 for relief of BPH symptoms.
%20in%20Check.jpg) Fish oil. A study examined how the essential fatty acids EPA and DHA affected SHBG levels in men 43 to 88 years of age.77 After controlling for other variables, the researchers concluded that both EPA and DHA decreased levels of SHBG in middle-aged and elderly men.
Fish oil. A study examined how the essential fatty acids EPA and DHA affected SHBG levels in men 43 to 88 years of age.77 After controlling for other variables, the researchers concluded that both EPA and DHA decreased levels of SHBG in middle-aged and elderly men.
Protein. While adequate protein consumption is vital to maintaining muscle mass, it is also important in maintaining testosterone levels. A study examined the relationship between diet and SHBG, and found that diets low in protein in men 40‒70 years old may lead to elevated SHBG levels and consequently decreased testosterone bioactivity.78
Natural Products to Support Sexual Function
Muira puama. Muira puama, Ptychopetalum olacoides, grows in the Amazon region of Brazil. It is considered an aphrodisiac and an effective treatment for impotence. It has been studied by Jacques Waynberg,79 a prominent medical sexologist at the Institute of Sexology in Paris. In one of his studies, men with loss of libido received 1.5 grams/day of muira puama for two weeks. Sixty-two percent rated the treatment as having a dynamic effect, and 52% with erectile dysfunction rated the treatment as beneficial. In another study, muira puama treatment was given to 100 men, aged 18 years or older, with impotence and/or loss of libido. A significantly increased frequency of intercourse was reported in 66% of the men. Of the 46 men  who complained of loss of desire, 70% reported libido intensification. The stability of erection during intercourse was restored in 55% of men, and 66% of men reported a reduction in fatigue. Other reported beneficial effects included improved sleep and morning erections.
who complained of loss of desire, 70% reported libido intensification. The stability of erection during intercourse was restored in 55% of men, and 66% of men reported a reduction in fatigue. Other reported beneficial effects included improved sleep and morning erections.
Maca. Maca has been used among indigenous people in the Andes region for centuries. It is a reputed aphrodisiac and fertility enhancer. Peruvian researchers conducted a randomized, placebo-controlled, double-blind study on a small group of men aged 21‒56. Results showed that, versus placebo, maca improved subjective reports of male sexual desire. Subjects consumed either 1,500 mg or 3,000 mg of maca, or placebo, for three months. After eight weeks, improvements were noted in sexual desire among the subjects who consumed maca.80
L-carnitine. L-carnitine is an amino acid derivative that may be more active than testosterone in aging men who have sexual dysfunction and depression caused by an androgen deficiency. Both testosterone and carnitine improve sexual desire, sexual satisfaction, and nocturnal penile tumescence, but carnitine is more effective than testosterone in improving erectile function, nocturnal penile tumescence, orgasm, and general sexual well-being. L-carnitine was also more efficacious than testosterone for treating depression.81
Natural Products to Support Prostate Health
 Indole-3-carbinol (I3C). I3C protects against dangerous estrogen metabolites and subsequent prostate cancer. An adequate intake of I3C, through vegetables such as broccoli, Brussels sprouts, and cabbage, or via supplements, may be very helpful for aging men in both keeping undesirable estrogen metabolites such as 16-alphahydroxyestrone in check and decreasing their risk of prostate cancer. Studies have demonstrated that I3C increases the ratio of 2-hydroxyestrone to 16-alpha-hydroxyestrone. For men, this very well might mean a decrease in prostate cancer risk.82,83 In a study that examined the association of prostate cancer risk with estrogen metabolism, the authors said, “results of this case-control study suggest that the estrogen metabolic pathway favoring 2-hydroxylation over 16-alpha-hydroxylation may reduce risk of clinically evident prostate cancer.”84
Indole-3-carbinol (I3C). I3C protects against dangerous estrogen metabolites and subsequent prostate cancer. An adequate intake of I3C, through vegetables such as broccoli, Brussels sprouts, and cabbage, or via supplements, may be very helpful for aging men in both keeping undesirable estrogen metabolites such as 16-alphahydroxyestrone in check and decreasing their risk of prostate cancer. Studies have demonstrated that I3C increases the ratio of 2-hydroxyestrone to 16-alpha-hydroxyestrone. For men, this very well might mean a decrease in prostate cancer risk.82,83 In a study that examined the association of prostate cancer risk with estrogen metabolism, the authors said, “results of this case-control study suggest that the estrogen metabolic pathway favoring 2-hydroxylation over 16-alpha-hydroxylation may reduce risk of clinically evident prostate cancer.”84
Pygeum. A bark extract from the native African cherry tree Pygeum africanum, has been used in Europe to treat BPH since 1960, and is currently the most commonly used therapeutic agent for this condition in France.85 One theory for the anti-BPH action of pygeum involves the conversion of testosterone to dihydrotestosterone (DHT), a potent testosterone metabolite that may exacerbate BPH, via the enzyme 5-alpha-reductase.86 A recent study identified that N-butylbenzene-sulfonamide (NBBS) was isolated from P. africanum as a specific androgen receptor (AR) antagonist. NBBS inhibits  AR- and progesterone receptor (PR)-mediated transactivation, as well as endogenous PSA expression and growth of human prostate cancer cells.87
AR- and progesterone receptor (PR)-mediated transactivation, as well as endogenous PSA expression and growth of human prostate cancer cells.87
Saw palmetto. In Europe, saw palmetto (Serenoa repens) has been used extensively as a drug for reducing symptoms of (BPH). Saw palmetto has multiple mechanisms of action: inhibition of 5-alpha-reductase; inhibition of DHT binding to the androgen receptor; reduction of the inflammatory component of prostate growth (by inhibiting COX-2 and an enzyme called 5-lipoxygenase); induction of apoptosis and inhibition of prostate cell proliferation.88-91 Its clinical benefits for prostate enlargement include reduced nocturnal urinary urgency,92 decreased residual urine volume in the bladder,93 and less discomfort from urination symptoms.94
Testosterone and Prostate Cancer: The Myth
 Historically, medical professionals suspected that testosterone replacement therapy would increase the risk of prostate cancer progression and recurrence.98 This fear made it standard practice for physicians to avoid testosterone replacement therapy in hypogonadal male patients that might otherwise have benefited from testosterone replacement.
Historically, medical professionals suspected that testosterone replacement therapy would increase the risk of prostate cancer progression and recurrence.98 This fear made it standard practice for physicians to avoid testosterone replacement therapy in hypogonadal male patients that might otherwise have benefited from testosterone replacement.
Remarkably, though, it appears that, in many cases, the opposite is true—lower levels of endogenous testosterone present a greater risk of prostate cancer than higher levels.95 A review by the National Institutes of Health revealed that, in men of advancing age, “…high testosterone levels are not associated with an increased risk of prostate cancer, nor are low testosterone levels protective against prostate cancer.”59
A review of data from 18 prospective studies compared serum concentrations of androgens and estrogens in 3,886 men with prostate cancer to 6,438 healthy controls. The results showed no  significant associations between risk of prostate cancer and sex hormone levels.60 A large cohort study published in 2020 supported the safety of testosterone therapy. Analysis of nearly 70,000 patients with a history of non-metastatic prostate cancer treated with radiation or surgery found that those who subsequently underwent testosterone treatment did not have an increased risk of cancer recurrence or mortality.98
significant associations between risk of prostate cancer and sex hormone levels.60 A large cohort study published in 2020 supported the safety of testosterone therapy. Analysis of nearly 70,000 patients with a history of non-metastatic prostate cancer treated with radiation or surgery found that those who subsequently underwent testosterone treatment did not have an increased risk of cancer recurrence or mortality.98
In more than 500 men diagnosed with prostate cancer (followed-up for over a mean of 8.7 years), high androgen levels were associated with a decreased risk of aggressive prostate disease compared with no change in risk of non-aggressive disease. Overall, levels of any steroid hormones (except estradiol) were not correlated with risk of aggressive prostate cancer.96
Abraham Morgentaler, an associate clinical professor at the Harvard Medical School, in his book Testosterone for Life, convincingly makes the case for the benefits and safety of higher testosterone versus the dangers of low testosterone. He also goes back to the original 1941 Nobel Prize-winning research97 about testosterone and shows how these data have been misinterpreted and unquestioned for over 70 years.
What You Need to Know: Optimizing Testosterone Levels in Aging Men
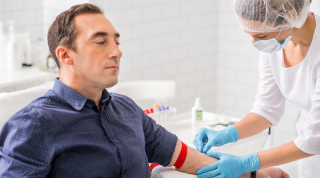 Testosterone, the chief male hormone, is essential for libido and erectile function, and plays a crucial role in mood, energy, bone health, and body composition.
Testosterone, the chief male hormone, is essential for libido and erectile function, and plays a crucial role in mood, energy, bone health, and body composition.- Testosterone levels decline with age, usually beginning in a man’s mid-30s. Diminishing testosterone levels have been linked with disorders such as depression, fatigue, obesity and cognitive decline.
- Low testosterone in men is strongly associated with metabolic syndrome, and may be a risk factor for type 2 diabetes and cardiovascular disease.
- Restoring testosterone to youthful levels offers men a wealth of health benefits, including benefits for heart health, body composition, mood, and memory.
- Bioidentical testosterone has not been found to have adverse effects on the healthy prostate gland—in fact, it may help improve prostate symptoms in men with low-normal testosterone levels. Testosterone therapy is contraindicated in men with prostate cancer.
- Regular blood testing can help you and your physician decide if testosterone therapy is right for you. Optimizing testosterone levels requires a multi-pronged approach that includes optimal diet, proper nutrition, nutritional supplements, exercise, and bioidentical testosterone.
Summary and Quick Facts
 Testosterone levels go down as we age and other hormones often fall out of optimal balance, too. Restoring youthful levels of testosterone and other hormones using bioidentical hormone replacement therapy can help support overall wellbeing.
Testosterone levels go down as we age and other hormones often fall out of optimal balance, too. Restoring youthful levels of testosterone and other hormones using bioidentical hormone replacement therapy can help support overall wellbeing.- Most men know that testosterone is important for health and performance, but many do not know that maintaining healthy levels of other hormones, like estrogen and DHEA, is also important. This protocol will help you learn about comprehensive hormone restoration and how it can support your health when combined with proper medical care, good diet and plenty of exercise.
- Supplementation with zinc and chrysin may help men maintain healthy hormone balance.
Material used with permission of Life Extension. All rights reserved.